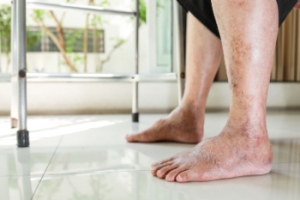
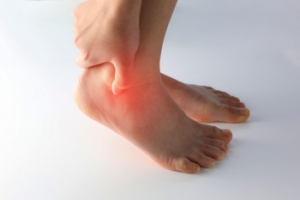
Understanding Your Health Through Your Feet
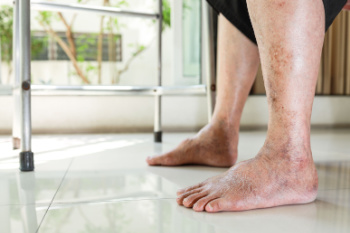
Your feet, often overlooked, hold valuable clues about your overall health. They serve as a mirror reflecting various underlying conditions that might otherwise go unnoticed. Paying attention to subtle signs can provide insight into your well-being. For instance, cold feet could indicate poor circulation, while dry, cracked skin might suggest dehydration or a nutrient deficiency. Swelling may signal issues with your heart, kidneys, or lymphatic system. Additionally, changes in toenails, such as discoloration or thickening, may hint at fungal infections or more serious ailments like diabetes or psoriasis. Moreover, persistent foot pain might not just be due to overuse but could signify conditions like plantar fasciitis or arthritis. Therefore, by observing and heeding the messages your feet convey, you can take proactive steps toward maintaining optimal health and addressing potential concerns before they escalate. After all, your feet are more than just the foundation of your body, they are valuable indicators of your overall well-being. If you have foot pain, it is suggested that you visit a podiatrist who may find underlying health issues and offer you specific treatment plans.
When dealing with systemic disease of the feet, it is extremely important to check the affected areas routinely so that any additional problems are caught quickly. If you have any concerns about your feet and ankles contact Dr. Joshua David Scoll from Pennsylvania. Our doctor will assist you with all of your podiatric needs.
Systemic Diseases of the Feet
Systemic diseases affect the whole body, and symptoms usually are displayed in the feet. This condition can make a patient’s ability to walk unbearable. Systemic diseases include gout, diabetes mellitus, neurological disorders, and arthritis.
Gout – is caused by an excess of uric acid in the body. Common symptoms include pain, inflammation, and redness at the metatarsal/phalangeal joint of the base big toe. Gout can be treated by NSAIDs to relieve pain and inflammation, and other drugs that lower the acid levels in the body.
Diabetes mellitus – is an increase in the level of blood sugar that the body cannot counteract with its own insulin. Failure to produce enough insulin is a factor in Diabetes.
Diabetes of the Feet
Diabetic Neuropathy – may lead to damaged nerves and affect the feet through numbness and loss of sensation.
Peripheral Vascular Disease – can restrict the blood flow to the feet, and often times lead to amputation of the feet.
If you have any questions please feel free to contact one of our offices located in Philadelphia, Bensalem, and Fairless Hills, PA . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Systemic Diseases of the Foot
There are several systemic diseases, or diseases that affect the whole body, that either display symptoms in the feet or affect the health of the feet. Common systemic diseases that affect the overall health of the feet, and the patient’s ability to walk comfortably, include gout, diabetes mellitus, neurological disorders, and arthritis, among others.
In gout, which is caused by an excessive buildup of uric acid in the body, the most common symptoms of pain, inflammation, and redness occur at the metatarsal/phalangeal joint at the base of the big toe. Any excess levels of uric acid crystallize and are deposited in tendons, joints, and surrounding bone and muscle tissue. Gout is commonly treated with NSAIDs to relieve pain and inflammation and other drugs to lower uric acid levels in the body. Gout most commonly affects those who are overweight, have low protein diets and lead a more sedentary lifestyle.
Diabetes mellitus is an increase in the level of blood sugar in which the body cannot counteract with naturally occurring insulin in the body. The three types of diabetes, Type I, Type II and Gestational Diabetes, are all signs the body is either not producing enough insulin or is not efficiently using the insulin that is produced. Gestational diabetes only affects women who are pregnant and have never, prior to pregnancy, exhibited symptoms of the disease.
There are two main issues that affect the feet that are commonly caused by diabetes. They include diabetic neuropathy and peripheral vascular disease. Diabetic neuropathy can lead to damaged nerves and affect the feet through numbness and loss of sensation. Peripheral vascular disease restricts the flow of blood to the foot and can, in extreme cases, lead to the necessity of amputating the foot. Peripheral issues that are caused by diabetes and can affect the foot include athlete’s foot, nail infections, corns, blisters, bunions, severe dry skin, plantar warts and ingrown toenails. These can all be attributed to the decrease of blood flow to the foot.
Neurological disorders and rheumatoid arthritis can also have severe impact on the health of the feet. Neurological disorders can affect the nerves in the main structure of the foot and cause loss of sensation and possible decreased muscle response. Rheumatoid arthritis can affect the bones and joint structures of the foot, making it impossible to walk normally without serious pain.
All systemic diseases that affect the foot can effectively be treated to minimize joint and muscle damage if they are diagnosed early and treated with medication and lifestyle therapy. Diabetes patients must monitor their blood sugar levels and work with their physician to keep their levels as close to normal as possible. Rheumatoid arthritis patients should work with their physician to ensure the proper medications are being taken to reduce the amount of damage to the joints of the body.
Recovery From a Foot Stress Fracture
Recovery from a foot stress fracture requires patience, diligence, and strategic care to facilitate optimal healing and prevent further injury. Begin by prioritizing rest and minimizing weight-bearing activities to alleviate stress on the affected foot. Elevate the foot above heart level to reduce swelling and promote circulation, aiding in the healing process. As symptoms improve, gradually reintroduce gentle stretching and strengthening exercises to rebuild muscle strength and flexibility. Consider incorporating low-impact activities like swimming or cycling to maintain cardiovascular fitness while avoiding undue strain on the healing fracture. Ensure proper nutrition, including adequate calcium and vitamin D intake, to support bone health and expedite healing. If you have a stress fracture that has affected your foot, it is suggested that you schedule an appointment with a podiatrist who can help you properly manage this condition.
Stress fractures occur when there is a tiny crack within a bone. To learn more, contact Dr. Joshua David Scoll from Pennsylvania. Our doctor can provide the care you need to keep you pain free and on your feet.
How Are They Caused?
Stress fractures are the result of repetitive force being placed on the bone. Since the lower leg and feet often carry most of the body’s weight, stress fractures are likely to occur in these areas. If you rush into a new exercise, you are more likely to develop a stress fracture since you are starting too much, too soon. Pain resulting from stress fractures may go unnoticed at first, however it may start to worsen over time.
Risk Factors
- Gender – They are more commonly found in women compared to men.
- Foot Problems – People with unusual arches in their feet are more likely to develop stress fractures.
- Certain Sports – Dancers, gymnasts, tennis players, runners, and basketball players are more likely to develop stress fractures.
- Lack of Nutrients – A lack of vitamin D and calcium may weaken the bones and make you more prone to stress fractures
- Weak Bones – Osteoporosis can weaken the bones therefore resulting in stress fractures
Stress fractures do not always heal properly, so it is important that you seek help from a podiatrist if you suspect you may have one. Ignoring your stress fracture may cause it to worsen, and you may develop chronic pain as well as additional fractures.
If you have any questions, please feel free to contact one of our offices located in Philadelphia, Bensalem, and Fairless Hills, PA . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Stress Fractures of the Foot and Ankle
Our bones are important aspects of our body and they are constantly changing. The heavier the workload for a bone, the more likely it is that calcium will be placed in it. When a bone isn’t used often, there won’t be much calcium within it. When stress from repetitive loads prevent the bone from being able to repair itself, cracks will start to form. Stress fractures are defined as cracks in a bone that result from repetitive force, such as overuse.
The most common cause of stress fractures is a sudden increase in intensity and duration of physical activity. For example, if you begin to run long distances without working your way into doing so, you will be more likely to develop a stress fracture.
Common symptoms of stress fractures are pain and swelling near the weight bearing area on the injured bone. When initial x-rays are performed, it is possible that the fracture will not show up. However, once the stress on the area continues, the damage will increase, and the fracture will be severe enough to show up on an x-ray. Certain parts of the foot are more likely to develop stress fractures than others. Areas that typically have these fractures are: the metatarsals, the navicular bone, the calcaneus, tibia, and fibula.
Since women are at an increased risk of developing osteoporosis, they are twice as likely as men to sustain a stress fracture. Additionally, old age causes a decrease in bone mineral density which is why elderly people are also likely to develop these fractures.
It is important for you to be professionally diagnosed by a podiatrist if you suspect you have a stress fracture, because there are other injuries that can easily be mistaken for a fracture. Sprains, strains, shin splints, plantar fasciitis, and Morton’s neuroma can all easily be mistaken for stress fractures in the foot. Your podiatrist will likely ask you a series of questions to determine what type of pain you are experiencing. These questions will help your doctor identify whether you have a stress fracture.
The best method of treatment for a stress fracture is rest. Additionally, a walking boot, cast, or crutches, will help rest the area that is injured. The typical healing time for stress fractures is 4-12 weeks, however this depends on which bone is involved.
An Overview of Tarsal Tunnel Syndrome
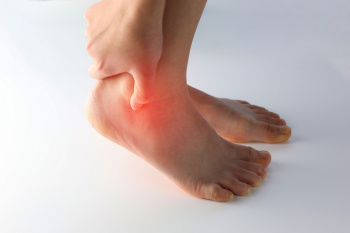
Tarsal tunnel syndrome, a condition affecting the feet and ankles, arises from compression of the tibial nerve as it passes through the tarsal tunnel, which is a narrow space on the inside of the ankle. Similar to carpal tunnel syndrome in the wrist, this ailment can lead to pain, tingling, and numbness in the affected area. The tibial nerve, responsible for sensory and motor functions of the foot and ankle, becomes compressed due to various factors such as injury, inflammation, or underlying medical conditions like arthritis or diabetes. Individuals with flat feet or those engaging in repetitive activities that stress the foot may also be at higher risk. Symptoms of tarsal tunnel syndrome include burning sensations, electric shock-like pain, and weakness in the foot. Prompt diagnosis and treatment, which often involves rest, can help alleviate symptoms and prevent further complications. If you have pain on the inside of your ankle, it is suggested that you consult a podiatrist who can accurately diagnose and treat tarsal tunnel syndrome.
Tarsal tunnel syndrome can be very uncomfortable to live with. If you are experiencing tarsal tunnel syndrome, contact Dr. Joshua David Scoll of Pennsylvania. Our doctor can provide the care you need to keep you pain-free and on your feet.
Tarsal Tunnel Syndrome
Tarsal tunnel syndrome, which can also be called tibial nerve dysfunction, is an uncommon condition of misfiring peripheral nerves in the foot. The tibial nerve is the peripheral nerve in the leg responsible for sensation and movement of the foot and calf muscles. In tarsal tunnel syndrome, the tibial nerve is damaged, causing problems with movement and feeling in the foot of the affected leg.
Common Cause of Tarsal Tunnel Syndrome
- Involves pressure or an injury, direct pressure on the tibial nerve for an extended period of time, sometimes caused by other body structures close by or near the knee.
- Diseases that damage nerves, including diabetes, may cause tarsal tunnel syndrome.
- At times, tarsal tunnel syndrome can appear without an obvious cause in some cases.
The Effects of Tarsal Tunnel Syndrome
- Different sensations, an afflicted person may experience pain, tingling, burning or other unusual sensations in the foot of the affected leg.
- The foot muscles, toes and ankle become weaker, and curling your toes or flexing your foot can become difficult.
- If condition worsens, infections and ulcers may develop on the foot that is experiencing the syndrome.
A physical exam of the leg can help identify the presence of tarsal tunnel syndrome. Medical tests, such as a nerve biopsy, are also used to diagnose the condition. Patients may receive physical therapy and prescriptive medication. In extreme cases, some may require surgery.
If you have any questions please feel free to contact one of our offices located in Philadelphia, Bensalem, and Fairless Hills, PA . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Tarsal Tunnel Syndrome
Tarsal tunnel syndrome is a condition in which there is a compression of the posterior tibial nerve. The posterior tibial nerve runs along the inside of the ankle into the foot. Tarsal tunnel syndrome is named for the tarsal tunnel, which is a thin space along the inside of the ankle beside the ankle bones. This space contains various nerves, arteries, and tendons, and includes the posterior tibial nerve. The tibial nerve is the peripheral nerve in the leg responsible for sensation and movement of the foot and calf muscles. In tarsal tunnel syndrome the tibial nerve is compressed, causing tingling or burning, numbness, and pain.
Common causes of tarsal tunnel syndrome involve pressure or an injury. Injuries that produce inflammation and swelling in or around the tunnel may place pressure on the posterior tibial nerve. Direct pressure on the tibial nerve for an extended period of time, sometimes caused by other body structures close by or trauma to the tibial nerve, can result in tarsal tunnel syndrome. Diseases that damage nerves, such as diabetes or arthritis, may cause tarsal tunnel syndrome. Those with flat feet are at risk for developing the condition, as the extra pressure and strain placed on the foot may compress the posterior tibial nerve.
Feeling different sensations in the foot at different times is a common symptom of tarsal tunnel syndrome. An afflicted person may experience pain, tingling, burning or other unusual sensations in the foot of the affected leg. Symptoms are primarily felt on bottom of the foot and/or the inside of the ankle. Symptoms can appear suddenly and may occur due to overuse of the foot.
To diagnose tarsal tunnel syndrome, your podiatrist may examine the foot and tap the posterior tibial nerve to see if symptoms surface. He or she may also order an MRI to determine if a mass is present.
Treating tarsal tunnel syndrome will depend on the decision of your podiatrist. Multiple options are available, however, and can include rest, ice, immobilization, oral medications such as anti-inflammatory drugs (NSAIDS), physical therapy, injection therapy, orthotics, supportive shoes, braces, and surgery.
Selecting Proper Running Footwear for Women

Selecting the right running shoes for women is essential for a comfortable injury-free running experience. When considering footwear, it is important to understand one's foot type and running style. Women should prioritize shoes that offer adequate support and cushioning, tailored to their unique needs. Assessing factors like arch height, pronation, and foot width helps to make the best selection. For individuals with low arches stability shoes provide support, while neutral shoes suit those with normal arches. Additionally, women with high arches benefit from shoes that offer extra cushioning and flexibility. The shoe's fit should feel snug yet allow room for natural foot movement. Investing in quality footwear that aligns with your specific biomechanics enhances comfort and reduces the risk of injury, enabling women to enjoy their runs to the fullest. If you are purchasing running shoes, it is suggested that you schedule an appointment with a podiatrist to select the appropriate pair.
You should always make sure your running shoes fit properly in order to avoid injury. For more information, contact Dr. Joshua David Scoll from Pennsylvania. Our doctor can provide the care you need to keep you pain-free and on your feet.
Choosing the Right Running Shoe for Your Foot Type
Improper shoe sizing can cause a myriad of problems for your feet. Shoes that don’t fit you properly can lead to muscular imbalances in your body, which can result in foot, knee, and hip injuries.
Tips for Finding the Right Running Shoe
- Make sure you have a thumb’s width of wiggle room between the end of your longest toe and the front of the shoe.
- There should be little to no slipping at the heel
- Don’t assume your size in one shoe brand will be your size in another
- Do not lace up your shoes too tightly
- Walk around in the store with your new shoes before you buy them
If you have any questions please feel free to contact our one of our offices located in Philadelphia, Bensalem, and Fairless Hills, PA . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Choosing the Right Running Shoe
Choosing the right running shoes for you is an important part of running. A good pair of running shoes will make the running experience more enjoyable for you and prevent potential injury.
Poorly-fitted shoes can increase the risk of injury in runners substantially. Common injuries from running with poor quality shoes include shin splints, sprained ankles, Achilles tendinitis, stress fractures, plantar fasciitis and more. This is due to the fact that bad shoes do not provide proper foot support, can increase pronation (how much the foot rolls when hitting the ground), have little to no cushioning, do not allow the feet to breath, and do not provide enough flex and rigidity in the right parts.
When looking for running shoes, first, determine where you will be running. If you are a trail runner, then pick trail shoes. If you run on concrete and asphalt, then regular running shoes are the best choice. When trying on shoes, its best to go at the end of the day as feet grow during the day and shrink after a night of sleep. Shoes should be more rigid towards the back of the foot while being more flexible up where the toes are. The toe box should provide enough room for the toes to move freely. The overall fit should be snug, not too tight but not too loose. A good pair of running shoes should also provide enough arch support for your foot type. If you experience overpronation or under-pronation while running, try to find a pair of shoes that will help correct this with different sole patterns. Finally, try to find a pair of shoes that allow the feet to breathe like nylon mesh or synthetic leather.
Don’t forget about the socks either. Socks that hold too much moisture can lead to athlete’s foot. Socks should be breathable so that your feet can air out and breathe. Synthetic socks wick away moisture like sweat. If you tend to run a lot, having a second pair of shoes that you can wear while you let the first pair air out is smart. Just don’t forget to replace your shoes after about every 300 to 500 miles.
Before you start running, it is advised to see a podiatrist to see if running is right for you. They can also offer good advice on how to run and what to look for in a pair of running shoes. If you have flat feet or poorly supported ones, they can also offer custom-made orthotics that will help give your feet the support they need.
Recovering From Ankle Replacement Surgery
Total ankle replacement, also known as total ankle arthroplasty, is a significant surgery aimed at relieving ankle pain. During the procedure, the surgeon removes parts of the shin bone, or tibia, and the top portion of the foot's highest bone, the talus, replacing the ankle with plastic or metal components. After surgery, you will likely have a cast, boot, or splint on your leg for approximately a month, and you will not be able to put weight on it immediately. You may need crutches, a walker, or a knee scooter during this time. It is important to have assistance at home during the initial recovery period. You will be discharged with bandages and stitches or staples, which your doctor will advise you on when to remove. Post-surgery, you may experience mild pain and swelling, for which your doctor may prescribe medication. Rehabilitation exercises, which are important for regaining strength and mobility, will continue for several weeks. Returning to work depends on individual recovery speed and job requirements, with certain movements or weight-bearing activities possibly restricted. If you have had your ankle replaced, it is suggested that you are under the care of a podiatrist who will provide personalized recovery steps for the most successful outcome.
In certain cases, in which the patient suffers from extreme pain or damage in a joint, joint replacement surgery may be deemed useful. If you have constant pain in a foot joint, consult with Dr. Joshua David Scoll from Pennsylvania. Our doctor will assess your condition and provide you with quality foot and ankle treatment.
What Is Joint Replacement Surgery?
Over time, joints wear down; this can be exacerbated by diseases and conditions. Joint replacement surgery, also known as arthroplasty, is when a damaged joint is surgically removed and replaced with a prosthesis. Prostheses, which can be made of ceramic, plastic, or metal, act as joints in lieu of an actual joint. One of the most prevalent causes for joint replacement is arthritis.
Arthritis in the Foot
Arthritis can occur in any joint in the body, including in the feet. Common types of arthritis in the foot are osteoarthritis, rheumatoid arthritis, and gout. The big toe is usually where arthritis occurs in the foot; this is known as hallux rigidus.
Joint Replacement Surgery in the Foot
The most common form of joint replacement in the foot is a first metatarsophalangeal (MTP) joint placement. MTP joint replacement surgery is designed to treat hallux rigidus. Surgery is not intensive, and recovery occurs within one to two months after the procedure has been done. Overall, joint replacement surgery is a safe and effective way to treat pain in the joint of the foot.
If you have any questions, please feel free to contact one of our offices located in Philadelphia, Bensalem, and Fairless Hills, PA . We offer the newest diagnostic and treatment technologies for all your foot care needs.